image source; aetrex.com
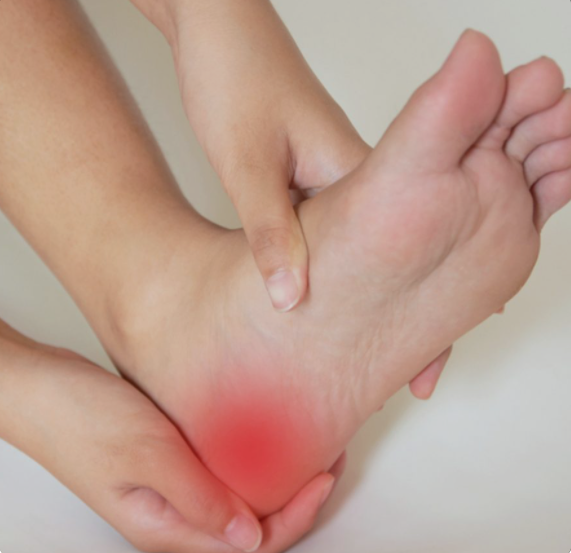
Heel pain, heel spurs, fasciitis are all layman’s words for what is known as Plantar Tendinopathy. The heel pain is like walking on pins with the first few steps getting out of bed in the morning or when arising from sitting during the day. Then after a few steps, the pain eases off … until the next morning.
What has been a problem since humans started walking on two feet, modern physiotherapy now understands the pain is due to a weakness developing in the foot muscle connective tissue. This connective tissue in the foot muscles can be weakened as a result of overloading caused by;
- Increasing the number of steps in a day – like when new exercise is started with the summer weather;
- Increasing impact exercise – like adding a hill to the normal walk, changing from walking to running etc..;
- A change in footwear – from supportive winter shoes to wearing thongs/bare feet in summer!
- A change in the standing surface – like moving into a house with concrete floors.
Once there has been an overload of the foot, microscopic changes in the muscle connective tissue occur. However, it takes a consistent 6 weeks of overload before the foot weakens enough so that heel pain is felt. The foot pain then hurts so much that you are forced to rest. Consequently, it settles in a few days. Then, you think,“Oh great, the foot has healed” and off you go again overloading a weak foot. Then, predictably, the foot is sore for a few days, you rest, it feels better. And on and on the cycle goes.
The classic example is my patient who developed heel pain when she changed jobs, going from standing 6 hours a day on carpet; to standing 8 hours a day on cement. Six weeks later her foot pain started. By changing her work shoes to sneakers, getting orthotics and sitting more in the day, the pain settled over the next few months. However, it would roar back again for a few crippling days with any unusual activity, like a day in bare feet with the kids at Adventure World, the morning after playing social basketball or the day after attending a wedding in high heels. By specifically strengthening her calf and foot muscles over 6 months, the connective tissue is stronger and able to tolerate more, so NO MORE HEEL PAIN!
So how can you fix the heel pain?
- Understand your current loading limit that won’t hurt the heel during the activity or the next day, then stick to that limit until you get stronger. Test yourself and learn how many steps a day you can comfortably manage, how far or fast you can run, how long you can stand for or how much time you can play on the basketball court in a game.
- Wear plantar tendinopathy friendly shoes. Choose shoes with a slight heel, that give a support to the arch, that have a good hold on the foot (ones that you don’t need to grip onto by clawing your toes!), have a bit of softness in the sole but are study enough not to be able to fold up into themselves. Sneakers are the obvious choice and thankfully they are in fashion.! But you can’t always wear sneakers: – Archies thongs, that we sell at the clinic, are great; men’s dress shoes are fine as long as the leather isn’t too stiff and wedges for women.
- Tendon specific Exercises – Physiotherapy can teach you the right exercises to perform at the right stage of your pain. It may take months to get stronger but this isn’t months of physio appointments – it is months of you doing your exercises to get stronger.
Summer is a classic time for persistent heel pain – plantar tendinopathy – to rear its very painful and ugly head. Book an appointment for Physiotherapy to teach you how to get strong and break the cycle of morning heel pain.