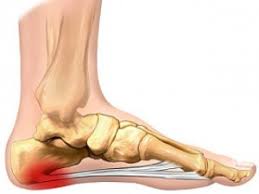
Heel pain is extremely common. Usual symptoms include feeling like walking on glass for the first few steps in the morning/after a period of sitting and an annoying dull heel ache with prolonged standing.
It used to be called plantar fasciitis and described as inflammation in the plantar fascia; treated with anti-inflammatory medication, foot rolling, calf stretches and orthotics. Pain directly depends on activity, so people would self-modify their exercise but it often just doesn’t go away. It can bother people for years.
“itis” is used to describe inflammation – think appendicitis.
”pathy” is used to describe disease that is not inflammatory.
Research has established that plantar fasciitis is not an inflammatory condition but it is in fact a change in the structure of the plantar fascia. Hence, the importance of the new name – Plantar Fasciopathy – and why Physiotherapy treatment has changed.
Plantar fasciitis is now known as Plantar Fasciopathy, and treatment has changed.
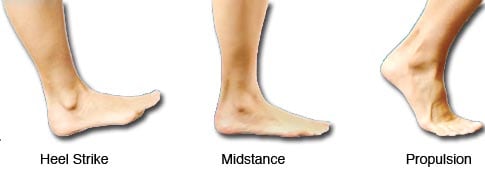
We now know plantar fasciopathy is the result of a change in impact loading of the leg resulting in altering the plantar fascia structure so it is less able to cope with impact force. The loading change can be too sudden increase in exercise (start training for a fun run and progress too quickly), a sudden decrease in exercise (reduced exercise due to sickness), change in shoes (barefoot or thongs all summer), change in surface (grass v cement v sand). And the list goes on, but there will be a change and the pain will come on 4-6 weeks after the change.
To cope with the forces of impact, the calf and plantar fascia are one unit and act like a spring.
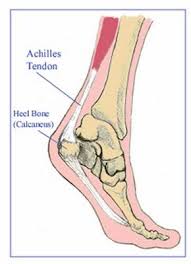
This spring has to cope with high forces:
- Walking; 3 x body weight
- Running; 9 x body weight
- Hurdling; 18 x body weight
When there is plantar fasciopathy, the leg can no longer effectively spring and cope with the forces.
When the condition is dominated by pain, isometric exercise is performed. This means a strong pain free contraction with no movement.
The heel pain should reduce within 1-3 weeks with this exercise.

When pain is controlled then the exercise progresses to weighted calf exercises. Increases have to be slow, with rest days in between this heavy loading phase. Remember weights transferred through the spring complex in the leg need to build up to > 9 x body weight in runners.


Rehabilitation back to preferred impact exercise takes 2-6 months depending on the exercise aim. The Physiotherapists at Active Solutions treat heel pain following the tendon degeneration model.